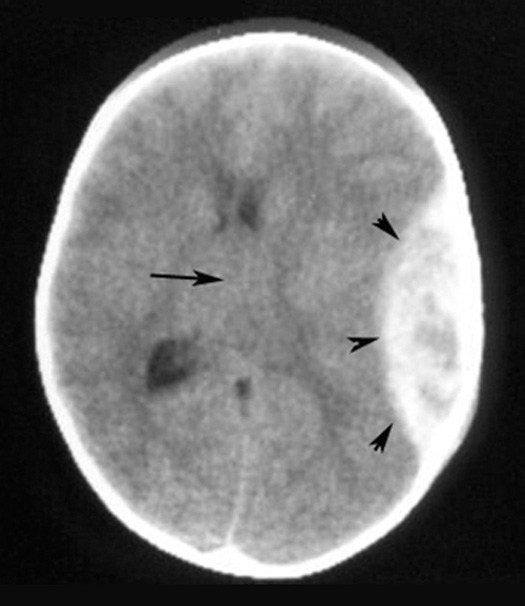
Figure 1
Epidural Hematoma
- Epidural hematoma is defined as collection of blood between the inner table of the skull and the dura.
- Common etiology is head trauma. More common in children as the dura is not as well fixed to the skull as in adults.
- Fracture line across the middle meningeal artery groove is noted on skull X-rays in 85-95% cases and, therefore, commonly located in the temporoparietal and parieto-occipital regions.
- Patient may present with classic lucid interval with initial period of loss of consciousness followed by a lucid interval of asymptomatic period with subsequent neurological deterioration leading to coma.
- Treatment is an immediate neurosurgical evacuation as the hematoma is result of an arterial bleed.
Pre-contrast CT findings of epidural hematoma:
- Biconvex in shape
- Acute blood is hyperdense (30-80 HU)
- Does not cross suture line, thus localized
- Mass effect due to hemorrhage and edema
Case 1:
CT brain of a child following trauma.
Imaging findings:
Figure 1 : Pre-contrast CT
-
Arrowheads point to localized epidural hematoma that is biconvex in shape.
-
Arrow points to midline shift.
Subdural Hematomas (SDH)
Subdurals are classified by the time to clinical presentation as acute, subacute or chronic.
Acute subdural: (0-2 days) Blood in acute stage appears hyperdense in a pre-contrast CT scan.
Chronic subdural: Chronic hematoma appears hypodense (lucent) as the cellular elements dissolve. Blood products are absorbed with time (after two weeks) and change to clear liquid. It now appears as dark or hypodense in a pre-contrast CT scan.
subacute subdural: In the subacute phase (between 3-14 days) it is isodense with brain and can easily be missed.
Subdural Hematomas (SDH)
- Subdural hematoma is defined as a collection of blood between the dura and the arachnoid.
- Common etiology: Head trauma (child abuse), coagulopathy.
- SDH is caused by movement of the brain relative to the skull, as in acceleration-deceleration type of injury, resulting in tearing of a cortical vein coursing within the subdural space. SDH is more common in patients with brain atrophy as the superficial veins are stretched over greater distance and are therefore more prone to rupture with rapid head movement.
- SDH is more common than epidural hematoma.
- SDH is usually caused by injury to veins. Thus clinical signs can be delayed, whereas epidural hematoma is the result of an arterial bleed.
- SDH is classified as acute, subacute and chronic by CT imaging. The hyperdense acute subdural evolves into isodense subacute subdural, and finally into hypodense chronic subdural hematoma (hygroma).

Figure 2
Acute Subdural Hematoma (0-2 days old)
Case 2:
Imaging findings:
Figure 2: Pre-contrast CT
- Patient with history of recent fall.
- Acute subdural hematoma covering the right cerebral hemisphere (yellow arrows) is seen.
- Blood in acute stage appears hyperdense in pre-contrast CT scan.
- Acute subdural hematoma is crescentic in shape (yellow arrows). Medial margin is not convex as in the epidural hematoma.
- Acute blood is hyperdense (CT density 30-80 HU).
- Acute subdural hematoma crosses suture lines, thus spreads diffusely over the brain surface (yellow arrows).
- Can cause significant mass effect with midline shift leading to brain herniation. White arrow points to mild compression of the right lateral ventricle with slight midline shift.

Figure 3
Chronic Subdural Hematoma (> 3 weeks old)
Case 3:
Imaging findings:
Figure 3: Pre-contrast CT
- Bilateral chronic subdural hygromas (yellow arrows) producing slight compression of the adjacent cortical sulci (white arrows).
- As the blood clot further liquefies, the subdural appears hypodense by CT imaging and reaches close to fluid density of cerebrospinal fluid within the cortical sulci/ventricles thus reaching the chronic stage (hygroma).
- Can be asymptomatic or can gradually increase in size leading to brain herniation.

Figure 4
Bilateral subacute Subdural Hematoma
Case 4:
Imaging findings:
Figure 4: Pre-contrast axial CT
- There are bilateral subdurals (arrow heads) isodense with the brain due to the gradual loss of density of blood.
- On close examination you see that the sulcal markings do not reach the surface of the skull, due to the intervening subdural collection.
- Arrowheads point to subdurals separating the brain surface from the skull.
- There is no midline shift due to bilaterality of subdurals.

Figure 5
Subarachnoid Hemorrhage (SAH)
- Defined as blood within the CSF subarachnoid space, it likely results from tears of small subarachnoid vessels either spontaneously or post trauma.
- SAHs classically present as atypical headaches which are abrupt in onset and severe ("worst headache of my life").
- Spontaneous subarachnoid hemorrhages are most often caused by rupture of arterial aneurysms which releases blood directly into the CSF. The most common cause of SAH overall is trauma.
- This rapidly increases intracranial pressure.
Subarachnoid Hemorrhage and Subdural Hemorrhage in a patient with head trauma.
Case 5:
Imaging findings:
Figure 5 : Pre-contrast axial CT
- Arrowheads point to subarachnoid blood in the sulci and SA space.
- Black arrow points to subdural blood.
- Normal sulci are filled with low density normal CSF and appear dark. Sulci filled with blood appear hyperdense.
- White arrow points to shift of midline to right.

Figure 6
Intracerebral Hemorrhage (ICH)
- Clinical effects of intracranial hemorrhage vary, many patients exhibit impaired consciousness.
- The most common causes of ICH are hypertension, trauma, rupture of aneurysm, rupture of AVM, tumor related hemorrhage, bleeding diatheses, illicit drug use and amyloid angiopathy in elderly.
Acute Intracerebral Hematoma
Case 6:
60 year-old patient with melanoma.
Imaging findings:
Figure 6 : Pre-contrast axial CT :
- Acute intracerebral hematoma within the right temporal lobe (arrow) with surrounding edema (E). Hounsfield units in the range of hemorrhage (68 H. U.).
Hemorrhage is from metastatic melanoma bleed. Acute hematoma is seen on non-contrast imaging as an area of high density.

Figure 7
- Most common in premature infants. Most intraventricular hemorrhages occur in the first 72 hours after premature birth.
- In adults it is often due to traumatic brain injury.
- Blood clots can block the flow of cerebrospinal fluid and cause hydrocephalus.
Intraventricular Hemorrhage
Case 7:
Thalamic tumor, resulted in marked degree of hydrocephalus requiring shunt catheter placement. Hemorrhage followed placement of the shunt.
Figure 7: Pre-contrast axial CT findings of shunt induced intraventricular hemorrhage:
- T: Thalamic tumor
- Arrow points to the shunt catheter
- V: Intraventricular blood
- Arrowheads point to normal CSF within the left lateral ventricle

Figure 8
intracerebral Hemorrhage extending into ventricles
Case 8:
Post op non-contrast CT brain study done after recent craniotomy. Post op CT demonstrates hemorrhage within the deep frontal lobe that has ruptured into the left lateral ventricle.
Imaging findings:
Figure 8. Pre-contrast axial CT
- Left deep frontal lobe hemorrhage (H) that has ruptured into left lateral ventricle (V).
- Arrowheads point to edema (arrowheads). E is edema.
- Yellow arrow points to displaced craniotomy flap from brain herniation (red arrows).
- Small white arrow points to compressed left lateral ventricle.
Systematic evaluation of imaging study in suspected cases of intracranial hemorrhage
Make sure that you are looking at non-contrast CT head.
Look for hyperdense lesion. Hemorrhage, calcium and contrast appear hyperdense in CT. Hence we need to look at non-contrast CT not to confuse contrast to hemorrhage.
- Locate the site of hemorrhage (ventricle, sulci, brain parenchyma, peripheral surface of brain, etc).
- Describe the shape of the density (round, biconvex, crescentic, etc).
- Look for edema around the hemorrhage manifested as hypolucent area.
- Look for midline shift and brain herniation.
- Look for fracture skull and soft tissue hematoma as patients may fall down and sustain head injury.
Your report should reflect that you evaluated these points.